Our team is staffed with experts who have 300+ total years of experience in the TPA and health insurance industry. We personalize our services to meet your needs. And because we are working 24/7, CXC is a round-the-clock extension of your own team for your operations and IT needs. We consistently manage the intricacies of increasingly complex FSA and HRA plans, freeing your team up to provide even better customer service.
...The support that we get with CXC, the real-time availability, helping us become available 24/7 in the processing arena...the caliber of people, the non-turnover...we seem to have gotten it right with CXC. - Services Manager, Large Third Party Administrator



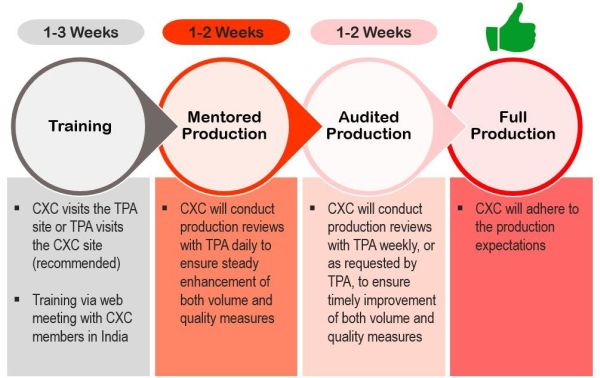

The CXC team has deep domain expertise in processing benefits claims. We cater exclusively to TPAs and can help you verify and adjudicate even the most complicated, manual HRA and FSA claims.

CXC's bookkeeping and payroll experts offer a personalized and flexible approach to your accounting/payroll data entry and processing needs. Our experts will work within your current software systems.

CXC's team of COBRA process experts will process insurance premium information and qualified beneficiary applications to ensure COBRA compliance for all your clients.
CXC offers debit card enrollment services. We help TPAs with the processing of benefit card applications, manual data entries and adjudication of benefit card claims. We also manage additions, changes, and terminations in the TPA system.
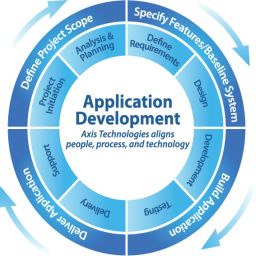
Our team of highly skilled developers is engaged during all stages of your software development life cycle. We help companies develop new products, leading the design, testing, implementation, and maintenance across various technology platforms.

CXC provides the following application maintenance services:Corrective/Adaptive/Preventative Maintenance, Testing, and Production Activities.




